In a race against time: modern stroke care
07.05.2026
This year's "Stroke Awareness Day" on May 10 is being held nationwide under the motto "I can feel what you can't see". The German Stroke Foundation wants to draw attention to the invisible consequences of a stroke, as four out of five strokes have hidden after-effects such as rapid fatigue, memory problems or speech disorders. In Germany alone, an estimated 1.2 million people live with impairments caused by a stroke.
A stroke, also known as a cerebral apoplexy, is not a uniform clinical picture. Depending on the cause, it is either a cerebral infarction or a cerebral hemorrhage. A cerebral infarction is caused by a vascular occlusion, whereas a cerebral haemorrhage is caused by a burst vessel in the brain. Factors favoring a stroke are high blood pressure, diabetes, lipometabolic disorders, obesity and smoking. However, psychological factors such as depression or stress can also be triggers. Many of these risk factors are exacerbated by a lack of exercise.
According to Deutsche Schlaganfall-Hilfe, around 270,000 people in Germany are affected by a stroke every year. Of these, more than 60,000 die as a result. This makes strokes one of the most common causes of death in Germany. Experts assume that the number of incidents will increase by more than 30 percent by 2040.
The first few minutes make all the difference
The most common symptoms of a stroke include sudden loss of vision, speech and language comprehension, paralysis and numbness, dizziness and very severe headaches. In the event of a stroke, a very small window of time often determines the health consequences, which is why the overriding principle in stroke medicine is "time is brain". The emergency services should be called as soon as a stroke is suspected, as a lack of blood flow to areas of the brain can lead to permanent damage to the brain.
This makes it all the more important to recognize typical warning signs in people in everyday situations at an early stage and to act immediately in an emergency. The FAST test, an acronym for Face, Arms, Speech and Time, is a simple guide. A crooked corner of the mouth, an arm that cannot be raised and impaired speech quickly provide certainty.

Innovations from the field
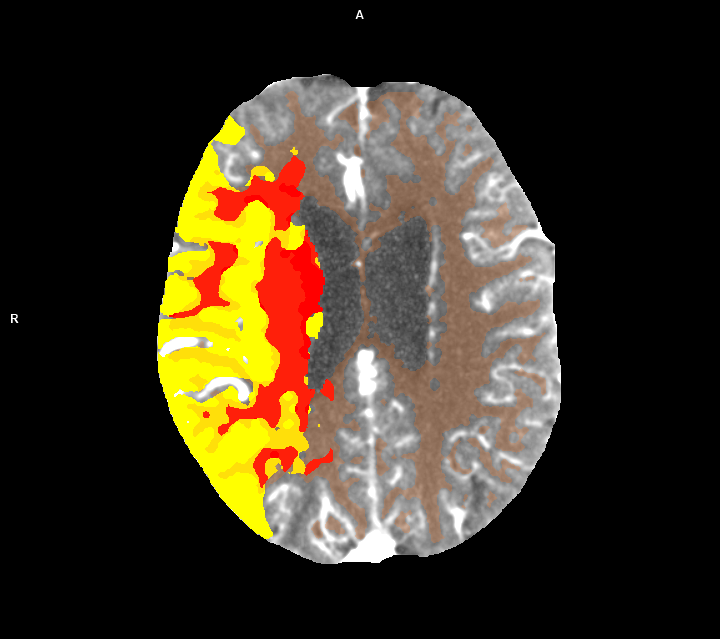
Today, almost twice as many people survive a stroke as 30 years ago. This development is mainly due to structural and technological advances in care. There are now over 350 certified stroke units in Germany, which guarantee highly standardized treatment. "These are specialized hospital wards that focus entirely on the treatment of acute strokes. Neurologists, specially trained nursing staff, physiotherapists and speech therapists work closely together here and there is seamless monitoring," explains Prof. Dr. Jan Liman, Chief Physician of Neurology at Nuremberg Hospital. At the same time, modern imaging has fundamentally changed treatment. High-resolution CT and MRI technologies make it possible to determine the cause of the stroke within a very short time and identify the brain tissue (penumbra) that can still be saved. "This has a direct impact on the speed of treatment," says Dr. Michael Scheuering, Head of Interventional Radiology at Siemens Healthineers.
The fact that stroke medicine is constantly evolving is due not least to the close integration of clinical experience, research and technological innovation. In Bayern Innovativ's Health Partner Network, players from medicine, science and industry are also working at precisely these interfaces - with the common goal of further improving the care of stroke patients. These include, for example, Nuremberg Hospital as a central service provider and Siemens Healthineers as an innovation leader in the field of medical imaging.
New care structures save time
This claim is particularly evident at Nuremberg Hospital. As a maximum care hospital, the clinic treats around 2,000 strokes a year, making it one of the largest stroke centers in Germany. The speed of the processes is what counts for the success of the treatment.

"The aim of a stroke unit is not to lose any time in the first hours and days after a stroke," explains Prof. Dr. Jan Liman, Head of Neurology, and continues, "rapid diagnosis, targeted therapies and early rehabilitation improve the chances of recovery and minimize consequential damage". How this principle is put into practice can be seen in the day-to-day work of the stroke unit. Here, specialized procedures and interdisciplinary cooperation interlock seamlessly, while heart rhythm, blood pressure and breathing are monitored around the clock.
Modern imaging is a central component of the closely timed procedures. "Modern imaging is at the heart of stroke care," emphasizes Liman. Procedures such as computer tomography and magnetic resonance imaging show within a very short time whether there is a vascular occlusion or a hemorrhage. "It is the imaging that determines the therapy," says Liman.
In order to further accelerate processes, Nuremberg Hospital is also working on new care approaches. One example is the so-called "one-stop" principle, in which patients with severe strokes, especially after occlusions of large cerebral vessels, are taken directly to an angiography room. There, imaging and treatment take place immediately one after the other. "This saves valuable minutes," explains Liman - a time saving of up to half an hour, which can be crucial, particularly in the case of severe strokes, so that patients suffer fewer disabilities and functional limitations. This approach is also being scientifically investigated: Together with the University Hospital Basel, Nuremberg Hospital and its Paracelsus Medical University (PMU) are leading the Europe-wide "GET-FAST" study, which began in 2025. The aim is to test whether patients recover better if imaging and treatment take place in the same room according to the "one-stop" principle.
The fact that effective stroke care is a team effort is evident along the entire care chain. "Good stroke care often starts before the hospital," says Liman. Accordingly, coordination between the ambulance service, emergency department and stroke unit is crucial - they must be closely networked. "Collaboration with other clinics is also important, for example when patients are transferred to a supra-regional center for special procedures." Here, telemedicine networks make it possible to "quickly integrate expertise, for example by sharing the results of imaging and the patient's clinical examination live via video".
The interface between imaging, processes and therapy is where it becomes clear how closely medical requirements and technological developments are linked. Clinical practice places clear demands on speed and precision - and thus also forms the basis for innovations in medical technology.
Technology as an accelerator
While hospitals such as Nuremberg Hospital are testing new care models, industry is providing the technological basis for them. Siemens Healthineers is developing solutions that combine diagnosis and therapy even more efficiently and thus accelerate the treatment pathway.
The role of imaging has changed fundamentally in recent years. "The key lies in the combination of speed, image quality and automation," explains Dr. Michael Scheuering, Head of Interventional Radiology. While diagnostics used to focus primarily on differentiating between bleeding and ischemia, it is now an integral part of the entire care chain.

"Thanks to modern CT and MRI technologies, we can assess much more precisely how much brain tissue is already irreversibly damaged and how much can still be saved," says Scheuering, adding, "Imaging has become faster, more robust and more informative. Automated evaluations, standardized protocols and digital workflows ensure that decisions can be made in the shortest possible time.
Artificial intelligence is also playing an increasingly important role. "Today, AI is an important partner in emergency diagnostics at various levels: it speeds up, standardizes and reduces the workload," says Scheuering. At the same time, the decision-making authority remains clearly with the doctors.
Another approach to gaining time is to move diagnostics closer to the patients. "Mobile stroke units enable significantly earlier diagnosis in the treatment pathway and allow treatment to begin immediately," says Scheuering. This can significantly shorten the time to treatment.

In addition to imaging, digital solutions also help to speed up processes. "Digital solutions and networking are key building blocks for fast and coordinated stroke care," emphasizes Scheuering. Image data, findings and analyses can now be shared across locations and enable close cooperation between all those involved.
Working together for better care
The examples from the network show how different the approaches to improving stroke care can be - and how much they benefit from each other. While clinical partners develop and evaluate new treatment processes, technological innovations create the conditions for faster and more precise decisions.
Especially in such a time-critical field as stroke medicine, it is clear how important this cooperation is. The Health Partner Network of Bayern Innovativ brings together precisely this expertise. Here, partners from different areas work together to further improve care - with the clear aim of saving more lives and sustainably improving the quality of life of those affected.